Voices in Global Surgery: Putting Mothers at the Centre of Safe Surgical Care in Kenya
"I have to respect them. I have to work for them." Meet Mary Mungai, a Nurse Anaesthetist in Kenya whose belief that the patient is the ultimate boss is transforming the quality of maternal surgical care across East Africa.
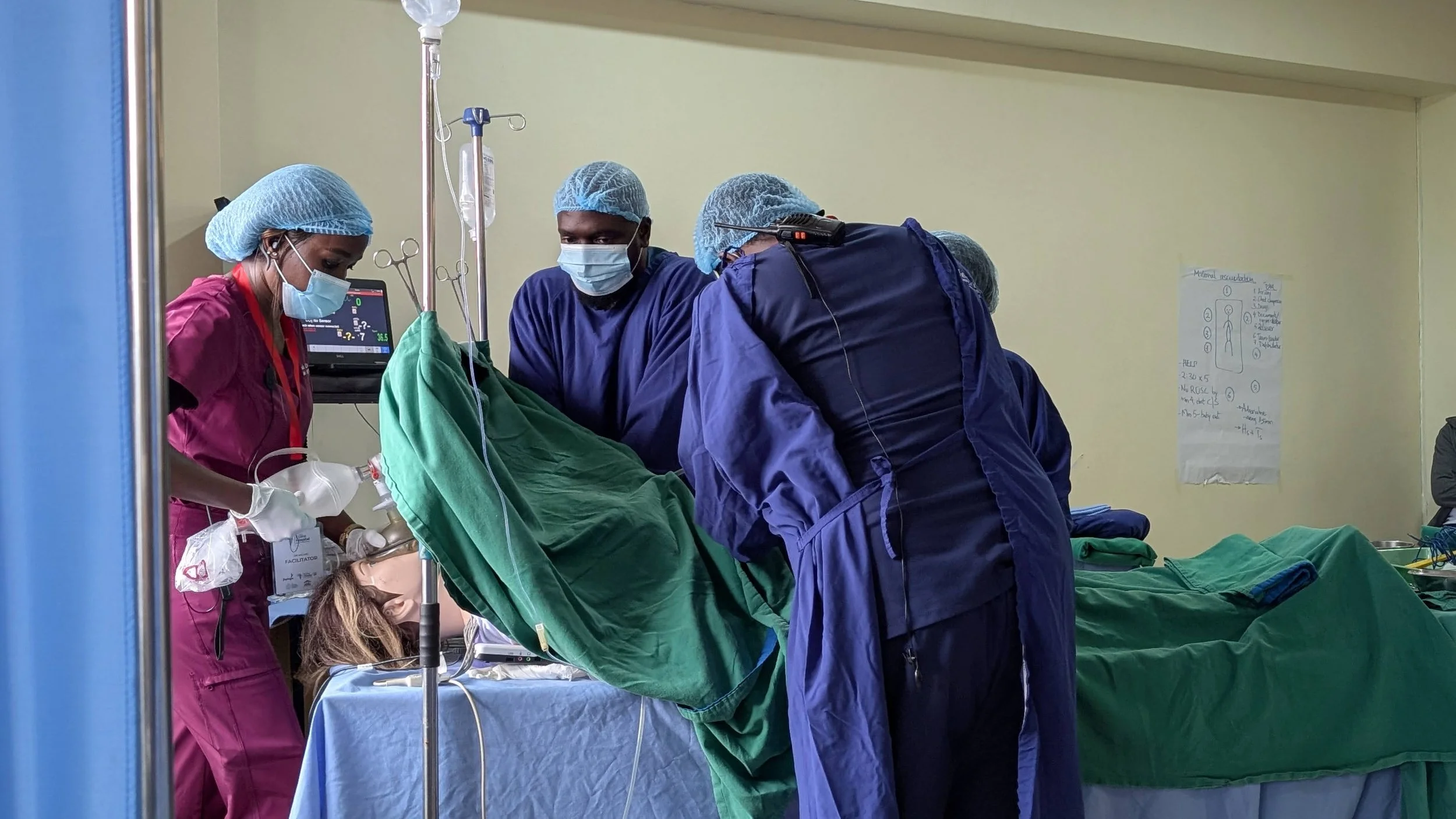
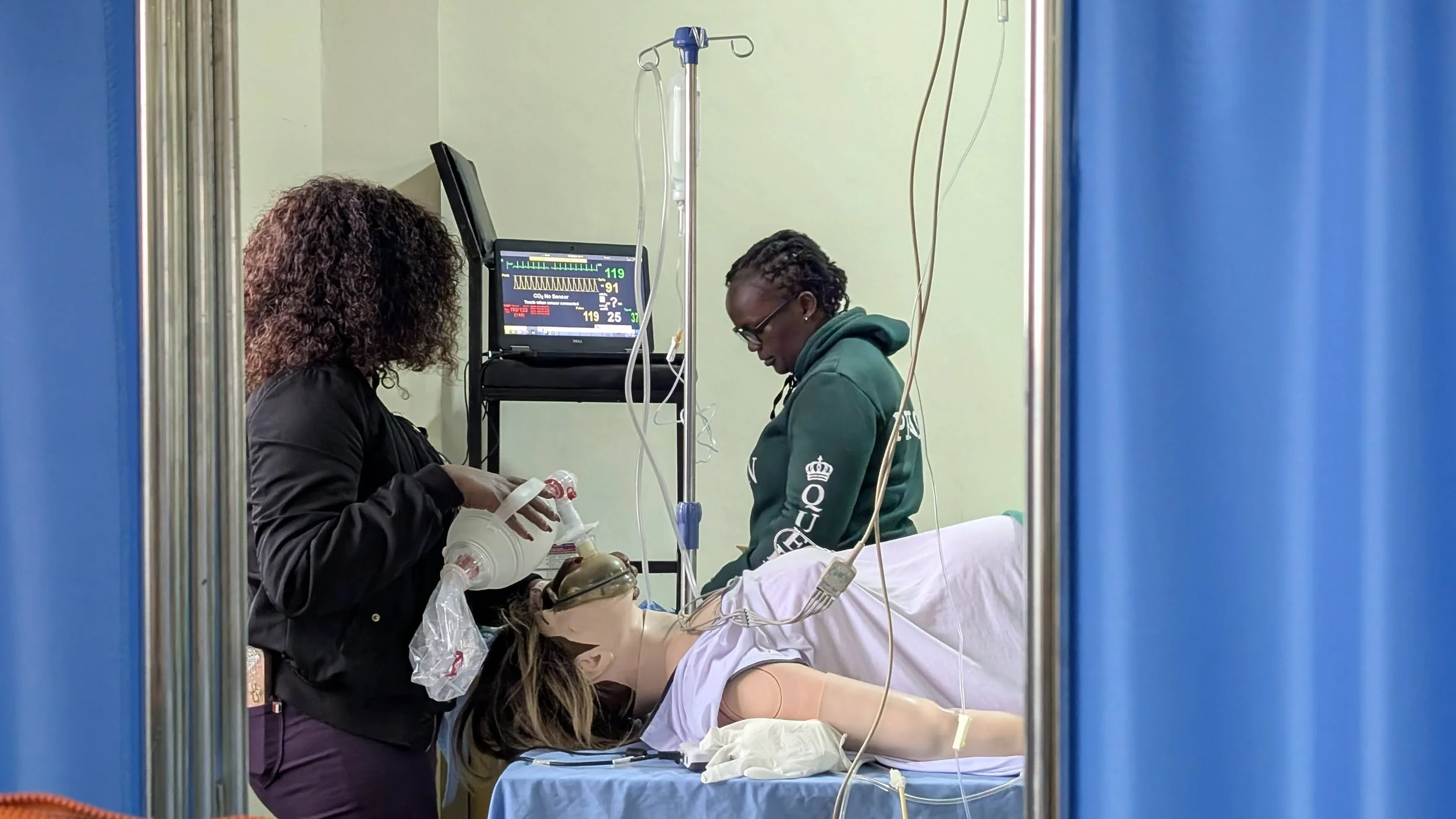
A surgical team engages in a hands-on obstetric simulation in Nakuru County to strengthen teamwork and emergency response skills.
A Career Dedicated to Improving the Quality of Surgical Care
In many parts of Kenya, childbirth remains a moment of both hope and risk. For Mary Mungai, Nurse Anaesthetist at AIC Kijabe Hospital, maternal safety is not just a professional responsibility – it is a deeply personal mission rooted in the realities faced by women and families every day.
Working across Kenya, Uganda, and Tanzania, Mary has dedicated her career to improving the quality of obstetric and surgical care. Her efforts on the frontlines are deeply aligned with the Global Surgery Foundation's broader mission to close the surgical care gap by empowering local healthcare workers and strengthening regional health systems. At the heart of her work is a simple but powerful belief: when mothers are safe, families and communities are safe.
Mothers as the Backbone of Families
In many communities, a mother is the backbone of the household – feeding children, ensuring they go to school, and holding families together. When a mother dies or is left with severe complications, the impact extends far beyond the hospital walls. “If she dies, the children may have no one to advocate for them,” Mary explains. “They may lose education, lose their future. This is not just about one life – it’s about generations.”
“At the heart of her work is a simple but powerful belief: when mothers are safe, families and communities are safe.”
Even when mothers survive childbirth, poor-quality care can leave lasting consequences. Babies who survive severe birth asphyxia may live with lifelong disabilities, placing enormous physical, emotional, and economic strain on families.
Hands-on neonatal simulation training ensures the best possible outcomes for newborns.
Quality of Care Goes Beyond Clinical Skills
Through Mobile Obstetric Simulation Training (MOST), Mary and her colleagues travel to health facilities to train multidisciplinary teams – surgeons, anesthetists, nurses, midwives, and medical officers – together. MOST places strong emphasis on teamwork, communication, leadership, and respect – non-technical skills that are essential during obstetric emergencies, where seconds can mean the difference between life and death.
“People are taught how to operate but nobody teaches them how to work together”
“In a crisis, everyone cannot be a leader,” Mary says. “You must identify one person to lead the team, communicate clearly, and respond quickly. This approach is a critical component of the Obstetric Safe Surgery in Nakuru County (OSS) Nakuru project, which aims to strengthen surgical systems by improving safety culture, teamwork, and standardised practices across facilities.
"Silence can kill." By running through high-pressure emergency scenarios on maternal simulators, multidisciplinary teams in Nakuru build the communication and clinical skills needed when seconds count.
Respectful Care Determines Whether Women Return
“When a woman comes to give life, that moment should be very respectful,” she says. “How you address her, the privacy you give her, the language you use – all of this determines whether she will come back to the hospital.”
For Mary, quality care is inseparable from respectful maternity care. The way women are spoken to, listened to, and treated during childbirth shapes their trust in the health system. In settings where communities have only recently begun to trust facility-based deliveries, disrespectful or dismissive care can undo years of progress. “Women agreed to come to hospital because we told them it was safer,” Mary reflects. “So, when they come, how do we treat them?”
“When a woman comes to give life, that moment should be very respectful.”
The Surgical Safety Checklist in action
A cornerstone of both MOST and the OSS Nakuru project is the consistent and correct use of the WHO Surgical Safety Checklist. For Mary, the checklist is far more than a piece of paper – it is a tool that empowers teams, flattens hierarchies, and protects patients. “Before we start, we introduce ourselves,” she explains. “In teaching hospitals, there may be many people in theatre. Do you know who they are? In a crisis, who do you address?” The checklist creates space for accountability and respectful challenge, even across professional hierarchies.
“I can say, ‘Doctor, I think we are losing blood,’” Mary says. “I say it respectfully, but I say it clearly. Silence can kill.”
She recalls a moment when a surgical swab count did not add up. Despite assurances that everything was correct, the team refused to close the patient until the missing swab was found. “We stayed until we found it,” she says. “If we hadn’t, that patient could have lived with severe infection or even died. This is how serious safety is.
Healthcare professionals in Naivasha proudly display their certificates after completing training for the Obstetric Safe Surgery (OSS) project in Nakuru County.
“My boss is the patient. I must respect them.”
At the centre of Mary’s work is a simple but powerful idea. “My boss is the patient,” she says. “Not the hierarchy, not the system.” That patient may be poor, barefoot, unable to read or speak English – but their dignity is unchanged. “They matter. They are human beings,” she says. “I must respect them, reassure them, and work for them.”
Looking Ahead With the OSS Nakuru Project
As the OSS Nakuru project continues, Mary is hopeful about its potential to create lasting change. “I’m excited to see teams using the checklist and talking to each other,” she says. “But this must go beyond training – it must become our culture.” For her, sustainability lies in shared ownership and passing knowledge forward.
“I only have two hands,” Mary reflects. “But if I impact someone else, they go on and continue the work. And that’s how we save many mothers.”
Voices in Global Surgery
Meaningful progress requires listening to those who know it best: the people with lived experience. Their unique expertise is irreplaceable when it comes to understanding and fixing the gaps in quality surgical care. In this series, we highlight the voices of those most affected to explore the critical barriers, challenges, and opportunities in achieving safe surgical care for all. Explore the series: article 1 | article 2 | article 3
About this Project
The Obstetric Safe Surgery - Nakuru County Project (OSS Nakuru) is a targeted intervention designed to improve maternal and perinatal outcomes for women across Nakuru County, Kenya. This project strengthens the local health system by implementing a hub-and-spoke training model to build surgical team capacity, improving referral networks, and enhancing data quality for decision-making. It is implemented by the Global Surgery Foundation (GSF) and Jhpiego, in partnership with AIC Kijabe Hospital and in close collaboration with the Ministry of Health of Kenya and the Nakuru County Government.
About the Funding & Implementation
This project is supported by SURGfund, the pooled financing mechanism of the Global Surgery Foundation (GSF). SURGfund is the world’s only pooled catalytic funding mechanism for strengthening surgical care systems. In addition to SURGfund financing, GSF provides strategic implementation support to ensure long-term sustainability.
Keep engaged with us!
Learn more about this project
Donate to support this project
Sign up with your email in the footer to receive updates
Your Next Article
The International Committee of the Red Cross (ICRC) and the Global Surgery Foundation (GSF) have joined forces to expand access to war-surgery training through SURGhub. Read More